Part One in a Two-Part series on Interventional Pulmonology and Diagnostic Imaging
The healthcare industry, and medicine, are constantly evolving and innovating.
One of the relatively new fields in pulmonology medicine is interventional pulmonology (IP), which utilizes endoscopy and other tools and techniques to diagnose and treat lung and chest conditions.
IP procedures are provided by pulmonologists (lung specialists) who receive extra training, cardiothoracic and other surgeons.
Procedures in interventional pulmonology in some cases may help avoid more invasive surgery. For example, prior to the development of IP, surgeons had to perform chest wall surgery to biopsy lymph nodes in the chest. IP offers less invasive procedures with a flexible bronchoscopy.
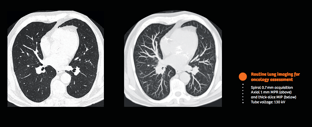
Acquisition and interpretation of images at point of care, in real-time, is essential to enable clinical decision-making.
Interventional pulmonologists can also perform lung or lymph node biopsies during a bronchoscopy by introducing a needle or forceps to collect small tissue samples from either the lung or lymph node. The tissue samples can be used to detect infection, cancer and other conditions. For some cancer patients, this type of biopsy often identifies the spread of cancer to nearby lymph nodes, which can prevent additional surgery. It can also help in choosing the best course of treatment for their condition.
The specialist also could perform a bronchoalveolar lavage during a bronchoscopy, by injecting sterile water through the bronchoscope into a segment of the lung. The fluid is then suctioned out and sent for tests. This procedure can help in diagnosing infection, cancer, bleeding, etc.
However, even flexible bronchoscopy aided by bronchoalveolar lavage didn’t offer the highest sensitivity possible, especially with smaller lesions. Today, computed tomography (CT) guidance can increase sensitivity and specificity, especially with larger, malignant, peripheral nodules.
Innovations in diagnostic imaging, such as endobronchial ultrasound, have revolutionized IP assessment of pulmonary nodules and lung cancer staging; it’s even less invasive and highly accurate and has increased the importance of the interventional pulmonologist’s role in the diagnostic assessment of thoracic diseases.
Other procedures performed in interventional pulmonology include:
- Airway or bronchial stent. Advanced cancer or some other conditions can compress bronchi (airway tubes). Blocked bronchi can result in breathing difficulties, cough, even pneumonia. A wire mesh stent is inserted into the constricted bronchus. When it’s expanded, it opens the bronchus, relieving the symptoms caused by the constriction.
- Balloon bronchoplasty. A deflated balloon is inserted into a section of atypically reduced airway. Symptoms are relieved when the balloon is inflated, expanding the airway. This procedure can be performed before inserting an airway stent to aid in expanding the bronchus.
- Rigid bronchoscopy. In rigid bronchoscopy, a long metal tube is inserted into a patient’s windpipe and main airways. The rigid bronchoscope’s larger diameter allows the use of more sophisticated surgical tools and techniques.
- Foreign object removal. Bronchoscopy (flexible or rigid) is the preferred IP method to remove inhaled foreign objects lodged in an airway.
- Pleuroscopy. Small incisions are made in the chest wall to advance a pleuroscope (a type of endoscope) into the chest cavity. The pleuroscope is moved around the chest wall and lung on one side to diagnose some conditions of the lining of the lung. Pleuroscopy also allows a view of the outside edges of the lung, which bronchoscopy cannot provide.
- Thoracentesis. A needle is inserted into the chest wall to drain fluid from around the lungs. A plastic catheter is sheathed over the needle, which is then removed. The excess fluid is suctioned out of the chest through the catheter.
- Pleurodesis. This IP procedure is performed in people with recurring fluid around the lungs.
- Indwelling pleural catheter. A pleural catheter is an alternative to pleurodesis for treating a recurrent pleural effusion.
- Bronchoscopic thermoplasty. Thermoplasty is an IP procedure for some severe asthma patients whose asthma can’t be controlled with medication.
Recent advances in technology play an increasing role in the detection and treatment of malignancies in airways, and are extending the reach of interventional pulmonology procedures:
- The endobronchial ultrasound system (EBUS) is a convenient, precise and safe method of assessing peripheral lung nodules. An ultrasound probe on the tip of a bronchoscope allows an IP to biopsy lymph nodes with more precision. It can significantly increase the likelihood of a correct diagnosis.
- Electromagnetic navigation bronchoscopy (ENB) and virtual bronchoscopic navigation (VBN) is an advanced system that provides quick and precise localization of peripheral lesions, especially in areas of the lung which would traditionally require invasive testing.
- Autofluorescence bronchoscopy, narrow-band imaging (NBI) and optical coherence tomography, are high-spatial, advanced airway assessment techniques that can provide for detailed evaluation of airways, and the potential of early detection of endobronchial malignancies.
Interventional pulmonology, and the accompanying technology, continue to evolve. And diagnostic imaging will remain critical to the field.
We’ll focus about the role of diagnostic imaging in interventional pulmonology in an upcoming blog!
Stay tuned for an upcoming Investing In You webinar focusing on bronchoscopy!







Comments