Cassling Blog
Stay informed with best practices and resources on the issues that matter most in imaging.
Imaging Implants with Confidence: Here’s What Technologists Should Know
After more than two decades in MRI and over 11 years teaching MRI physics, one thing has become clear to me: implant safety is one of the most misunderstood responsibilities we have as technologists. Every day, we balance patient comfort, diagnostic quality and safety in an environment where even small oversights can have... Read moreHow Echo IQ Transforms Heart Disease Diagnosis with Cutting-Edge AI
What does the future of heart disease detection look like? Professor Geoff Strange, Chief Research and Strategy Officer at Echo IQ and Professor of Medicine at the University of Sydney and Notre Dame, recently sat down with the Cassling team to discuss the game-changing capabilities of EchoSolv. EchoSolv, the... Read moreby Veronica Sapp in Imaging, cardiology
The Top Imaging Trends of 2024
2024 was a year of innovation across the imaging spectrum. When we reviewed our top articles of the year, it became clear that what resonated more than anything else were in-depth looks at technology, the cost of that technology, and the myriad other innovations changing the clinical conversation. Here are the top articles... Read moreRSNA 2024: AI Reaches Critical Mass
At the annual meeting of the Radiological Society of North America in Chicago, radiologists, technologists and assorted medical professionals from all around the country once again gathered to catch a glimpse of the latest technological breakthroughs in the radiology space. In the last couple years, artificial intelligence... Read moreWhat’s New in CT Systems and Scanner Technology: 2025 Edition
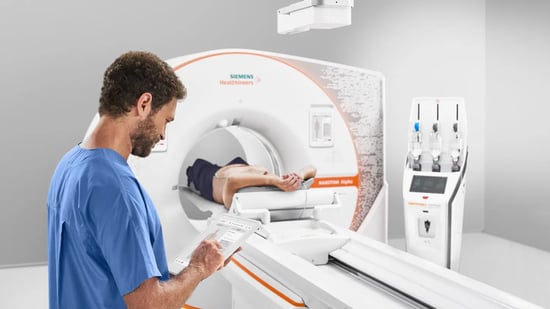
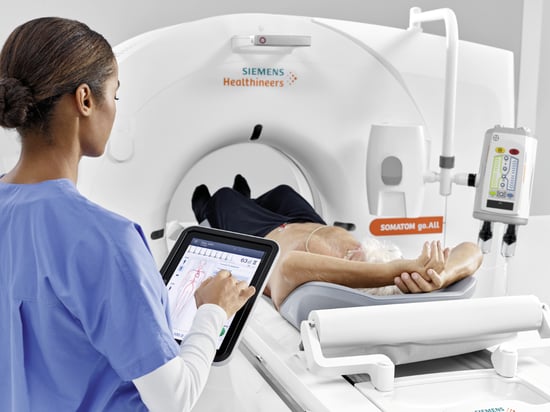
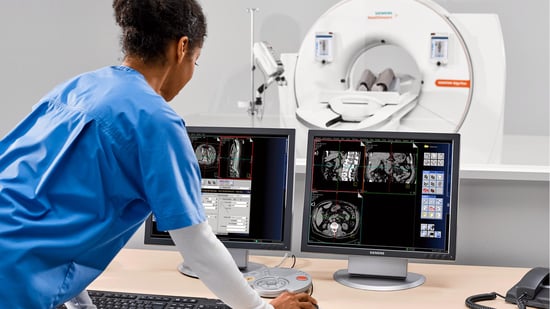
If it’s been a few years since your team has opted for a new Computed Tomography (CT) scanner, you might be surprised by the progress the technology has made. New best practices that seek to enhance the patient experience like never before are being deployed regularly not just in large health systems, but even in smaller... Read moreWhat’s New in MRI Technology — 2025 Edition
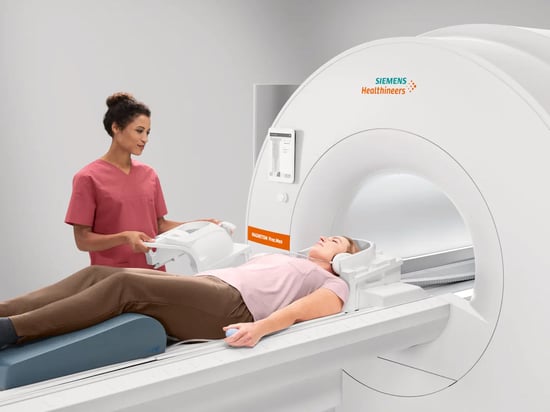
With so many technological advancements happening across all of healthcare, it’s easy to lose sight of the incredible evolution happening to one of the cornerstones of the hospital imaging experience: MRI. 2025 will continue to see a number of improvements to the MRI patient experience, the workflows of imaging teams and... Read moreHow to Tell When Imaging Equipment Has Reached End-of-Life (and How to Extend Its Value)
Like humans, medical imaging equipment shows signs of aging. But instead of creaky joints, wrinkles, or gray hair, the machinery gives other hints that it is wearing out and that it might be time for you to make a change. Here are five signs that your imaging equipment is approaching its last lap, plus tips on what you can... Read moreIs Your Equipment Helping or Hurting Patient Communication?
With existing scheduling backlogs, radiology technologists are feeling the pressure to move fast. While patient volumes have swelled, staffing challenges have left a less-than-optimal workforce with a bigger workload. A critical element of care can suffer on account of this pressure: patient communication. Effective... Read morePredictions and Hopes for Healthcare in 2024
As we head into the New Year, we’re starting to see some very positive trends in healthcare. Staffing within the healthcare space has roared back, outpacing basically every other industry. Drug prices continue to weigh on the average consumer, but new rules and negotiation policy have sought to bring some of those down.... Read moreAUC Program Penalty Phase Suspended Indefinitely: We Answer Your Frequently Asked Questions
UPDATE: As of Jan. 1, 2024, the Appropriate Use Criteria program will not be implemented in any capacity. A notice on the CMS website currently (1/4/24) reads: "As announced in the CY 2024 Physician Fee Schedule (PFS) Final Rule, effective January 1, 2024, CMS has paused efforts to implement the AUC program for... Read moreInnovative Imaging Technology Leads Top Trends of 2023
What a year it’s been! We continue to be amazed by the imaging teams around the country who commit so much of themselves to improving patient outcomes. It’s why we remain honored to help you celebrate your teams with free resources for National Rad Tech Week and Medical Ultrasound Awareness Month, and it’s why we strive... Read moreby Veronica Sapp in Imaging,
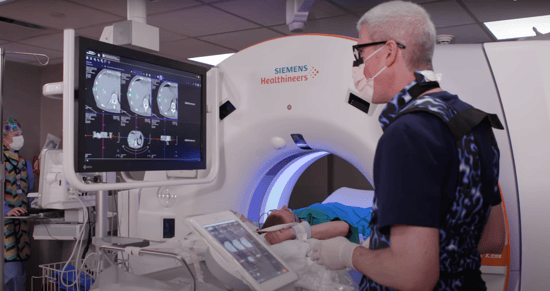
SOMATOM X.Cite + myNeedle Companion - Simplifying CT-Guided Intervention
Dr. David Lacey, Interventional Radiologist at Iowa Methodist Medical Center, a Cassling customer, details how myNeedle Companion on the SOMATOM X.cite helps simplify CT-guided interventions from start to finish. Dedicated in-room control options offer the flexibility to work as you prefer – with or without an assistant.... Read moreCassling's New Website Empowers Imaging Providers
Our new website is officially live! The Cassling website has been rebuilt from the ground up to improve your experience. When we launched our new vision for strengthening community healthcare earlier this year, it quickly became clear that we had work to do to convey the full scope of how we can help healthcare providers.... Read more10% Computed Radiography Reimbursement Cut in Effect: Get the Facts
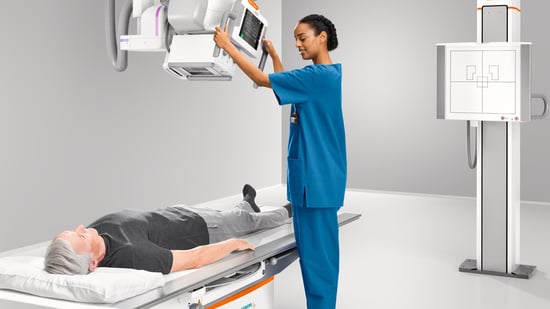
At the beginning of this year, a reimbursement cut came into effect that went largely under the radar, despite many providers still utilizing the system in question. For the past few years, providers of outpatient Medicare-eligible X-rays conducted on a computed radiography system experienced a payment reduction of 7% on... Read moreby Veronica Sapp in Imaging, X-ray,
Cardiac Imaging Systems Review: What's In, What's Out, and MRI's Big Moment
Interventional cardiologists have unique needs. The highly specialized nature of cardiology is such that you need special equipment and software to do your best work and improve clinical workflows, staff experience and, ultimately, patient outcomes. A new era of interventional cardiology is here, and with it comes new... Read moreby Mark Miller in Imaging, cardiology








.webp?width=550&name=MAGNETOM%20Sola%20Cardiovascular%20Edition%20(2).webp)
